
Geographic access to physiotherapy affects health outcomes
New spatial analysis of the geographic distribution of physiotherapists reveals healthcare inequities in Canada and Aotearoa New Zealand...
Spatial analysis illuminates geographic differences, proximity issues and access to resources. It’s a growing area of interest in health research for its ability to inform health policy and planning. The recent collaborative work of Drs Stephan Milosavljevic (PhD), Brenna Bath—professors in the School of Rehabilitation Science—and Tayyab Shah (PhD)—Geospatial Research Manager and Specialist with the Canadian Hub for Applied and Social Science Research (CHASR)—is at the forefront of spatial analysis methods as they apply to health services.
A recent visit from Dr Miranda Buhler (PhD) has added another strand to the research of Drs Milosavljevic and Shah. Based at Aotearoa New Zealand’s University of Otago School of Physiotherapy in Dunedin, Buhler is conducting a spatial analysis of the Aotearoa New Zealand physiotherapy workforce.
Like Canada, Aotearoa New Zealand has large, sparsely populated geographies alongside metropolitan areas; increasing socioeconomic inequality; a disastrous history of colonisation of indigenous peoples; with more rural populations, those with higher socioeconomic deprivation and people of indigenous ethnicity experiencing poorer health outcomes.
Disparities in outcomes and access for health conditions (such as musculoskeletal diseases, cardiovascular illnesses and neurological disorders) also exist in both countries where physiotherapy can play a major role. Identifying geographic accessibility to care is a key contributor to analyzing inequities in health. Yet the geographic distribution of the physiotherapy workforce across Aotearoa New Zealand remained unexamined, until Buhler’s research.
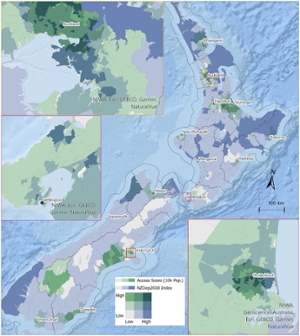
The geospatial 3-step floating catchment area (3SFCA) method is well suited to examining accessibility across both rural and metropolitan areas like those found in Aotearoa New Zealand and Canada. This method integrates demographic variables to gain a more granular view of where mismatches lie between supply and demand. With the collaboration and support of Milosavljevic, Shah and colleagues, Buhler conducted a 3SFCA analysis in the Aotearoa New Zealand context (see Figure 1).
Not unlike analysis of Canadian data, the team identified specific areas in Aotearoa New Zealand with high spatial inequity of physiotherapy accessibility, including areas with high proportion indigenous Māori population, Pacific population, high socioeconomic deprivation, and rural areas. These findings will inform local and national planning as the country’s new health system (Te Whatu Ora – Health NZ) evolves.
Buhler also met with Drs Sarah Oosman (PhD), Brenna Bath (PhD) and Stacey Lovo (PhD) from the School of Rehabilitation Science to hear firsthand the challenges and successes of working alongside First Nations communities to reinvent how healthcare can better suit the people it must serve.
“I am very grateful for the wonderful hospitality of Professor Steve and the School of Rehabilitation Science, and Dr Shah and the CHASR lab” said Buhler. “It has been a privilege to spend time among these amazing teams and to benefit from their remarkable experience and expertise in applying not only geographic methods, but also understanding the social context and dynamics of population and workforce data sets. I am excited about moving forward in this field and the continued benefits that collaboration brings.”
Buhler used a Māori proverb (whakataukī) to summarize her visit and the ethos underlying research to address healthcare inequities: Nāku te rourou, nāu te rourou, ka ora ai te iwi. “With your food basket and my food basket the people will thrive.” Working in isolation might result in survival, but working together can take people beyond survival and onto prosperity.
